Pelvic and Abdominal Rehabilitation Services
Pelvic and Abdominal Rehabilitation Services
Our team of physiatrists and physical therapists specialize in diagnosing and treating pelvic and abdominal health concerns for adults and children of all ages. Mary Free Bed pelvic and abdominal therapy offers comprehensive care to address a variety of conditions. Common therapies for pelvic and abdominal rehabilitation (PAR) include:
Pelvic Floor Therapy
Abdominal Muscle Therapy
Bowel Dysfunction Therapy
Pelvic Rehabilitation for Men and Women
Pelvic Rehabilitation for Pregnancy-Related Issues
Understanding Pelvic and Abdominal Rehabilitation
Pelvic and abdominal rehabilitation focuses on rehabilitating the muscles, ligaments, and joints of the pelvic region and surrounding areas.
This type of rehabilitation helps manage symptoms, relieve pain, and improve strength, mobility and function.


Common Symptoms of Pelvic Floor Dysfunction:
- Chronic or recurring pelvic and abdominal pain
- Musculoskeletal pain (hip, low back, sacroiliac joint, tailbone)
- Bladder and bowel incontinence
- Constipation
- A feeling of pressure or heaviness deep within the pelvis
- Painful intercourse
Who is at Risk?
Pelvic and abdominal concerns can affect women, men, and children. Symptoms may stem from:
Perinatal Pelvic Changes
Surgery (C-section, Hysterectomy, Bladder Suspension, Prostatectomy)
Trauma
Effects of Radiation to the Pelvis for Cancerous Conditions (Pelvic Radiation)
Neurological Disorders
Gender Affirmation Surgery
Pregnancy (Prenatal and Postpartum)
Changes Associated with Perimenopause and Menopause
Diastasis Recti (Abdominal Separation)
Treatment, Risks, and Benefits
In Mary Free Bed’s Pelvic and Abdominal Rehabilitation Program, physical therapists who specialize in pelvic and abdominal rehabilitation use noninvasive techniques to help manage symptoms, relieve pain, and improve strength, mobility, and function. Your personalized treatment plan may include:
- Instruction on behavioral techniques for bladder and bowel retraining
- Integration of manual therapy techniques
- Dietary modifications for bladder and bowel retraining
- Biofeedback to train/re-educate pelvic floor muscles
- Electrical stimulation
- Fitting for braces or supports
- Education on pain management strategies
- Postural and biomechanical education and training
- Therapeutic exercise for strengthening and conditioning
- Individualized exercise program
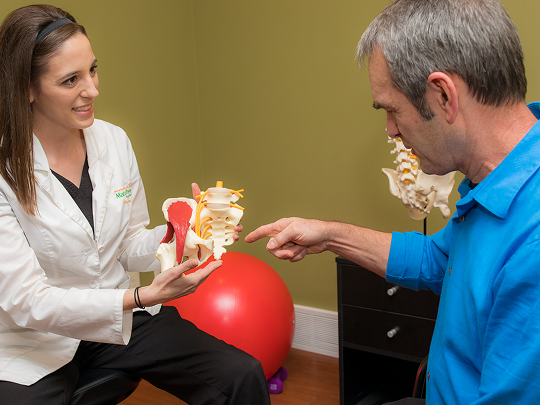
Pelvic and abdominal concerns can affect women, men – including adults, teen and children Symptoms may stem from:
- Perinatal pelvic changes
- Surgery (C-section, hysterectomy, bladder suspension, prostatectomy)
- Trauma
- Effects of radiation to the pelvis for cancerous conditions (or pelvic radiation)
- Neurological disorders
- Gender affirmation surgery
- Pregnancy (prenatal and postpartum
- Changes associated with perimenopause and menopause
- Diastasis recti (also known as abdominal separation)
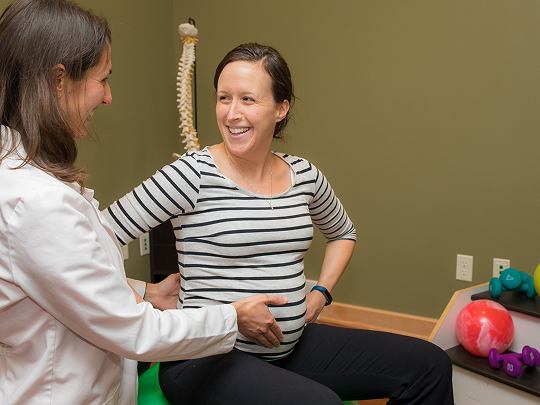
- Improved physical conditioning and muscle function
- Enhanced bladder and bowel control
- Reduced pain and discomfort
- Increased mobility and flexibility
- Greater independence and quality of life
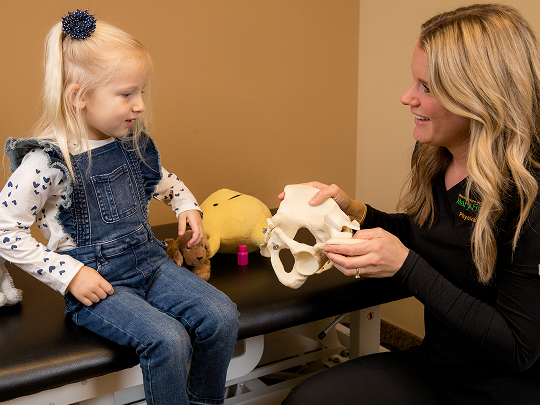
Protecting Your Health Through Pelvic and Abdominal Rehabilitation
Our comprehensive pelvic and abdominal rehabilitation services are designed to support a holistic approach to recovery.
By combining physical activities with education and support, we empower patients to regain independence and enjoy life through meaningful activities.
Frequently Asked Questions
Pelvic floor therapy is a specialized form of physical therapy designed to treat pelvic floor dysfunction, a common but often misunderstood condition affecting people of all ages and genders. The pelvic floor plays a critical role in bladder control, bowel function, core stability and sexual health. When these muscles aren’t working properly, symptoms can significantly impact daily life, but the good news is that pelvic floor therapy is highly effective.
This comprehensive guide explains what the pelvic floor is, how it functions, common symptoms of dysfunction and how pelvic floor physical therapy can help restore strength, coordination and confidence.
What is the Pelvic Floor?
The pelvic floor is a group of muscles and connective tissues located at the base of the pelvis. These muscles form a supportive sling that extends from the pubic bone at the front to the tailbone at the back and side to side between the sit bones.
The pelvic floor consists of three layers of muscle, each with a specific role in support, continence and movement.
Pelvic Floor Muscle Layers
Layer 1: Superficial Layer This outermost layer includes:
- Bulbocavernosus
- Ischiocavernosus
- Superficial transverse perineum
- External anal sphincter.
These muscles play an important role in continence and sexual function.
Layer 2: Middle Layer
This layer includes:
- Deep transverse perineum
- External urethral sphincter
In females, this layer also includes the sphincter urethrovaginalis and compressor urethrae, which help control urinary flow.
Layer 3: Deep Layer
The deepest layer provides the most structural support and includes:
- Coccygeus
- Levator ani group (puborectalis, pubococcygeus, iliococcygeus).
What Does the Pelvic Floor do?
The pelvic floor is essential for multiple body systems and works in coordination with the diaphragm, abdominal muscles and spinal stabilizers.
Key Functions of the Pelvic Floor
Pelvic Organ Support
The pelvic floor supports the bladder, uterus (or prostate), rectum and bowel, helping prevent pelvic organ prolapse.
Bladder and Bowel Control (Continence)
These muscles contract to keep the urethra and anus closed and relax to allow urination and bowel movements.
Relaxation and Elongation
Proper relaxation is just as important as strength. The pelvic floor must lengthen to allow comfortable urination, defecation and penetrative intercourse.
Core Stability and Pressure Management
The pelvic floor works with the core and diaphragm to stabilize the spine and regulate intra-abdominal pressure during lifting, coughing, exercise and daily movement.
Sexual Function
Pelvic floor muscles contribute to sensation, arousal, function and orgasm.
Common Symptoms of Pelvic Floor Dysfunction
Pelvic floor dysfunction can present in many ways. Common symptoms include:
- Urinary or fecal incontinence.
- Leakage with coughing, sneezing, laughing or exercise.
- Painful intercourse (dyspareunia).
- Pelvic, hip, low back, tailbone, abdominal or sacroiliac (SI) joint pain.
- Constipation or difficulty emptying bowels.
- Feeling of incomplete bladder emptying.
- Urinary urgency or overactive bladder.
- Pelvic pressure, heaviness or bulging.
- Pelvic organs prolapse (cystocele, uterine prolapse, rectocele, enterocele or vaginal vault prolapse).
- Endometriosis-related pelvic pain.
- Diastasis recti (abdominal separation).
What Causes Pelvic Floor Dysfunction?
Pelvic floor dysfunction typically results from muscle weakness, muscle tightness, poor coordination or a combination of these factors.
Pelvic Floor Weakness
Weakness may lead to:
- Bladder, bowel or gas leakage.
- Pelvic organs prolapse.
- Feelings of heaviness or bulging in the pelvic area.
- Reduced sexual sensation or satisfaction.
Common contributors include:
- Pregnancy and childbirth
- Surgery
- Aging
- Menopause and decreased estrogen.
Pelvic Floor Tightness
Tight or overactive pelvic floor muscles may cause:
- Constipation
- Difficulty starting urination
- Painful urination or bowel movements
- Painful intercourse
- Pelvic, hip or low back pain.
What to Expect During a Pelvic Floor Therapy Evaluation
A pelvic floor evaluation is thorough, individualized and patient-centered. Evaluations may include:
- Detailed discussion of symptoms, medical history and lifestyle factors.
- Posture, breathing, strength and movement assessment.
- External or internal pelvic examination (only with patient consent).
Internal exams are never required and are performed only if appropriate and agreed upon.
Types of Pelvic Floor Therapy Treatment
Pelvic floor therapy treatments are tailored to each patient. Treatment may include:
- Strengthening weak muscles, including pelvic floor muscle, hips, abdominals and lower back.
- Manual therapy and myofascial release.
- Stretching and relaxation techniques.
- Biofeedback and neuromuscular re-education.
- Breathing and pressure-management training.
- Education on posture, hydration, bowel and bladder habits.
Benefits of Pelvic Floor Therapy
Pelvic floor physical therapy can help patients achieve:
- Improved bladder and bowel control.
- Reduced pelvic, hip and back pain.
- Improved sexual comfort and function.
- Reduced prolapse symptoms.
- Increased core strength and stability.
- Improved confidence and less stress.
How to Find a Qualified Pelvic Floor Therapist
When searching for a pelvic floor therapist, look for:
- Clinicians with specialized pelvic health training and experience treating your specific symptoms.
- A professional, supportive environment.
- Someone who you can communicate with comfortably.
What causes pelvic pressure, bulging or feelings of something “falling out?”
These symptoms are often related to pelvic organ prolapse or pelvic floor weakness. Pelvic floor therapy can help manage symptoms and prevent progression. Even if additional medical treatment is needed, pelvic floor therapy helps improve strength and prevent further prolapse.
What is pelvic organ prolapse?
Pelvic organ prolapse occurs when pelvic organs descend from their normal position and move into the vaginal canal or anus.
What causes pelvic organs to prolapse?
Weakness in connective tissue and pelvic floor causes pelvic organs to prolapse. Common risk factors include pregnancy and childbirth (especially vaginal delivery), aging, menopause, decreased estrogen, heavy lifting, chronic coughing, straining, constipation and obesity.
Can pelvic floor therapy help pelvic organ prolapse?
Yes. Mild to moderate prolapse often responds very well to pelvic floor therapy. Even in more severe cases that may require additional medical intervention, therapy plays an important role to improve strength, habits and mechanics to support recovery and prevent future prolapse.
Why do I have constipation?
Constipation has many causes. Constipation can be related to diet, hydration, posture or pelvic floor dysfunction. A pelvic floor therapist can assess what may be contributing factors. Therapy treatment may include education, stretching, strengthening, relaxation and positioning techniques.
Can pelvic floor therapy help with straining or pain during urination or bowel movements?
Yes. The pelvic floor must relax fully to urinate or defecate. Difficulty relaxing these muscles can cause pain, straining or incomplete emptying. Pelvic floor therapy may focus on coordination, posture, stretching and relaxation strategies.
What is diastasis recti?
Diastasis recti is a separation of the abdominal muscles, commonly occurring during pregnancy. A pelvic floor therapist can assess if there is separation and guide safe recovery.
Why do I have tailbone, pelvic or abdominal pain?
These symptoms may be related to pelvic floor tightness, pelvic, hip or spine instability. Pelvic or abdominal pain is also a common symptom of pelvic organ prolapse. A pelvic floor therapist can identify contributing factors and provide treatment to improve these symptoms.
Am I drinking the right fluids?
Many people don’t drink enough water, or they may consume bladder irritants. Learning how to stay hydrated is often part of therapy.
How do I stop an overactive bladder?
You may have to learn to relax your pelvic floor and reduce bladder irritants. A pelvic floor therapist can help with this.
What causes urinary urgency or overactive bladder symptoms?
Urgency may be caused by pelvic floor tightness, poor mechanics or bladder irritation. Pelvic floor therapy can address all contributing factors.
Can I do too much exercise?
Yes. Exercising too much or progressing too quickly can increase symptoms. A pelvic floor therapist can help guide safe return to activity, especially postpartum or after surgery.
Can pelvic floor therapy help painful intercourse?
Absolutely. Pelvic floor tightness, weakness or poor muscle coordination can all contribute to pain with intercourse and can be treated with pelvic floor therapy.
Is pelvic floor dysfunction common?
Yes—it’s extremely common. Many people experience symptoms, but don’t talk about them because they’re embarrassed. Pelvic floor dysfunction is treatable and nothing to be ashamed of. Sharing symptoms helps providers give you the best care. They may also be able to provide you with resources and additional support.
Can I do pelvic floor therapy without an internal exam?
Yes. Internal examination is only one component of the assessment, and it’s never required. Many effective strategies can be used without internal exams. Your comfort and consent always come first.