Guest blog: Dr. James Hudson is medical director of the Pain Rehabilitation program. He’s specialized in the treatment and management of patients with chronic pain at Mary Free Bed for more than 30 years.
He leads a specialized team of doctors and therapists who use a rehabilitation approach to pain management. In this blog, Dr. Hudson discusses the history of fibromyalgia and treatment.
In 1990, the American College of Rheumatology, an association of arthritis specialists in the United States, published its first clinical diagnostic criteria for the diagnosis of fibromyalgia. American medicine previously had no agreed upon way of diagnosing this condition. We had been seeing patients with complaints of widespread pain and fatigue for whom none of our diagnostic tests could pinpoint a cause, and physicians and patients were left without knowing what was wrong or what to do about it.
Publication of clinical diagnostic criteria allowed for research into the condition. We could take patients who met the criteria and follow them over time to see what happened and to test whether any particular treatment was successful. We now have 29 years of research into fibromyalgia and have learned a great deal. We know, for instance, that this condition doesn’t shorten one’s life. There’s no sign of tissue damage no matter how long they’ve had the condition. It doesn’t attack organs, such as the liver, kidneys, lungs, brain or nervous system, or destroy joints or nerves.
In recent years, imaging studies using functional Magnetic Resonance Imaging (MRI) and Positron Emission Tomography (PET) have shown there are changes in the way the brain functions in patients with fibromyalgia compared to normal controls. Their nervous systems seem to be overly sensitized, responding to non-painful stimuli in ways we see in patients with more serious tissue damage. This has led researchers to see fibromyalgia as a central sensitization disorder. We find no pathology in the patient’s muscles, bones, ligaments or connective tissue, only changes in the way the nervous system functions.
There have been many drug trials in patients with fibromyalgia, and a few medications have shown improvements in symptoms compared to patients who were given placebo pills instead. These medications are duloxetine, gabapentin, pregabalin, tramadol, cyclobenzaprine and amitriptyline. The response has varied between patients. Many have significant side effects and stop treatment, and others feel worse. Some report less pain, less fatigue and better alertness.
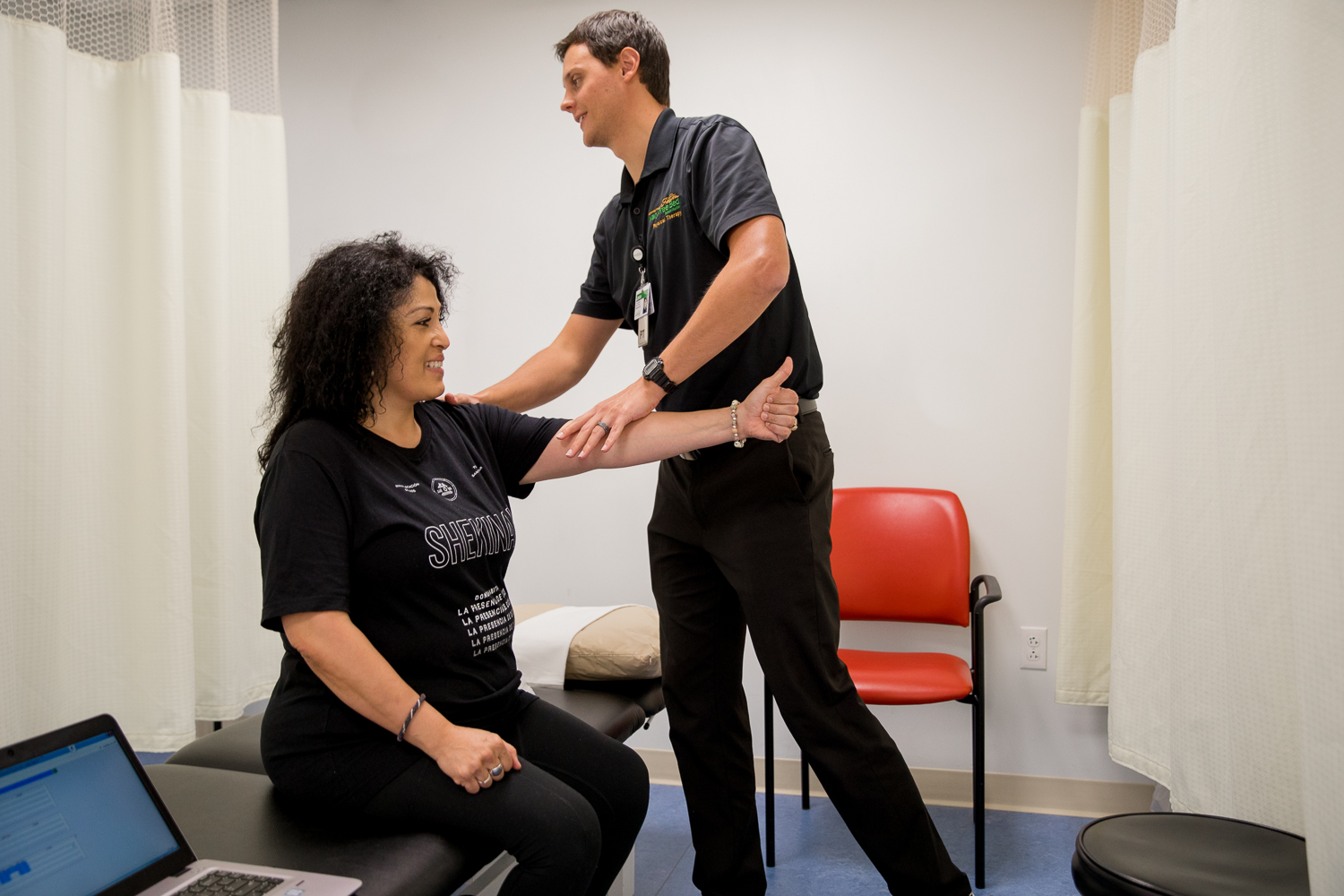
When the National Institute of Health looked at outcomes from treatment for fibromyalgia, it found the best results occurred in patients treated with multiple disciplines. This is what we offer in Mary Free Bed’s Pain Rehabilitation Clinic. Our physical therapists are experienced in treating people with widespread pain and fatigue, who have significant worsening of symptoms when they over-do exercise. They are careful and teach you to pace yourself. At the same time, they work with you to overcome fear of movement and help establish a regular routine of exercise and rest.
 Our team’s occupational therapists focus on your daily activities and the recreational and social activities important to you. We assess your most meaningful activities so you feel like you’re getting your life back and not just going through meaningless exercises.
Our team’s occupational therapists focus on your daily activities and the recreational and social activities important to you. We assess your most meaningful activities so you feel like you’re getting your life back and not just going through meaningless exercises.
The pain psychologist addresses the emotional impact of not only the pain but the way your whole life has been affected by this condition. This helps you recognize the role stress and emotions play in making your nervous system overly sensitive and all the additional symptoms this can create. Most importantly, it teaches you how to calm those emotions and manage stress in a way that allows your body to heal. This leads to being more intentional in the way we all respond to the ups and downs of life. It teaches skills such as mindfulness to calm ourselves and improve relationships, improve sleep and focus on living in a manner we’re proud of.
The medical providers in our program focus on making sure you’re on medications with good evidence for effectiveness, and try to eliminate any medications that interact adversely with each other or that cause more problems than they help. Our team communicates weekly to ensure that progress continues.
We’ve created a support group for patients who have completed one of our programs and are interested in providing and receiving support from other patients with similar diagnoses. We’re always here if you need additional care later.
We offer Pain Rehabilitation at four locations – Grand Rapids, Benzonia, Holland and Kalamazoo – so you can get the care you need close to home.