Brain Injury Rehabilitation
Brain injuries – whether mild or traumatic – are complex. Brain injury challenges and recoveries are unique to each person. At Mary Free Bed, we begin by understanding who you are – your motivations, goals, and what brings meaning to your life. Together, we take a comprehensive approach to move beyond the trauma of injury and toward healing.
Why choose Mary Free Bed?
Rehabilitation is vital to recovery after a brain injury. Research shows that starting rehabilitation as soon as possible leads to better outcomes.
Our specialized programs, extensive experience, and compassionate care make us a trusted partner on your recovery journey.


Specialty Brain Injury Accreditation
Our inpatient and outpatient Brain Injury Rehabilitation Programs are accredited by the Commission on Accreditation of Rehabilitation Facilities International (CARF). This rigorous process ensures the highest level of care from your physicians, therapists and nurses who specialize in brain injury rehabilitation and recovery.

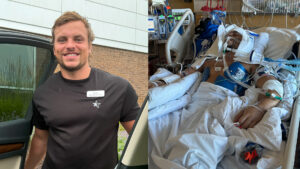
Memory, Speech & Strength: Jon’s Inspiring Story after a Traumatic Brain Injury
Your Brain Injury Recovery Journey at Mary Free Bed
Inpatient Rehabilitation: Comprehensive Brain Injury Care
We’ll help you or your loved one regain as much independence as possible while finding ways to successfully adapt to challenges. Our calming environment and supportive team are here to celebrate your successes and help navigate difficult days.
Personalized Therapy:
Your therapy program will be customized to your needs and tolerance, focusing on achieving the best outcomes.
Specialized Spaces:
Therapy gyms, including a low-stimulation environment, support strength and fine motor skill development. Private treatment spaces are available for speech-language therapy.
Daily Living Skills:
Practice essential tasks such as cooking, laundry, and cleaning in a simulated apartment setting.
Family Involvement:
Loved ones are encouraged to participate in therapy sessions and learn alongside you.

Outpatient Therapy
Whether you’re in the recovery phase of a concussion or seeking ongoing care after a traumatic brain injury, Mary Free Bed provides a full spectrum of care, including specialized therapy, home and community services and life-long follow-up care.
Our outpatient Brain Injury Clinic offers a range of therapy services, technology and treatment, whether you’re a graduate of our inpatient Brain Injury Program or you were referred by a physician for outpatient treatment. A thorough evaluation allows us to create a therapy plan to best meet your needs. The length of treatment can vary from a few sessions to a couple of months.

Care for a Lifetime
We’re committed to supporting you for as long as you need us. After completing inpatient care, we offer:

Specialty Services
To enhance your recovery, we coordinate access to services like:
- Wheelchair and Adaptive Sports Program
- Assistive Technology
- Driver Readiness Screening
- Spasticity Management
- Neuropsychology
- Motion Analysis Laboratory
- Post-Concussion Program

Community Resources
- Support Groups: Monthly support groups to connect with others managing brain injuries. Learn More
- Mentorship Opportunities: Pairing with experienced mentors who provide insight and encouragement. Learn More
- Adaptive Sports: Programs for all ages to rediscover the joy of movement. Learn More

Meet Your Brain Injury Rehabilitation Team
Your dedicated team includes specialists from various disciplines, all experts in brain injury rehabilitation. They work together to maximize your recovery and independence.
You and your family or caregivers are the most important members of the team. You’re encouraged to have an active role in your treatment plan and help set goals for your rehabilitation.
Frequently Asked Questions
Here are questions we often hear from patients who have experienced a brain injury. Talk with your treatment team about specific questions or concerns.
How long does it take for a brain injury to heal?
Recovery depends on the type and severity of the injury. Intensive rehabilitation helps maximize your independence and recovery potential.
How long will I stay at Mary Free Bed?
Your length of stay depends on your injury’s severity, current functionality, and progress. Patients typically stay anywhere from a few days to several weeks.
Can my family participate in my therapy?
Absolutely. Family involvement is encouraged to support your transition to independence, though therapists may occasionally ask family members to step back to ensure focus during sessions.
Why do I have problems swallowing?
Brain injuries can disrupt swallowing muscles or focus, leading to difficulties. A speech-language pathologist can assess and treat these challenges.
Why did my personality change?
Brain injuries can affect emotion regulation and behavior. This is a common, natural part of recovery, and we’re here to help you and your family navigate these changes.
Advanced Technology and Specialized Spaces
At Mary Free Bed, technology and innovative spaces play a critical role in your recovery:
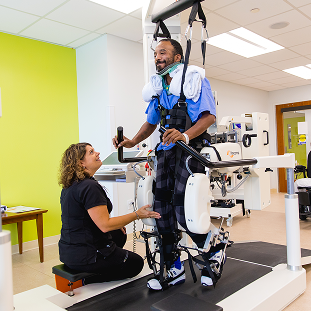
ZeroG and Lokomat® Pro
Ceiling-mounted systems and robot-assisted technology for safe walking therapy.